BACTERIA FACTS
The Dutch merchant and amateur scientist Anton van Leeuwenhoek (1632–1723) was the first person to observe bacteria and other microorganisms. Using single-lens microscopes of his own design, he described bacteria and other microorganisms (calling them "animalcules") in a series of letters to the Royal Society of London between 1674 and 1723.
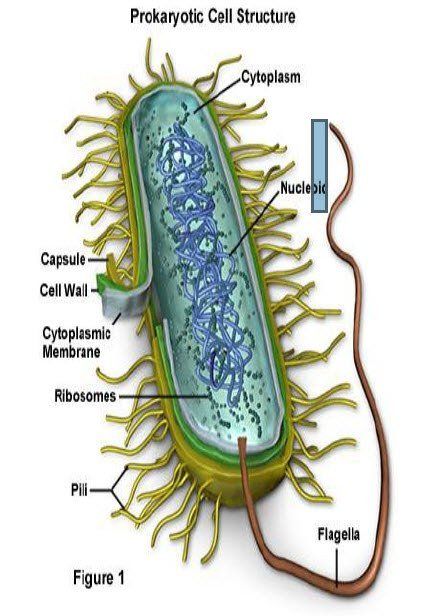
Bacteria are generally classified into three groups based on their shape. They are described as spherical (coccus), rodlike (bacillus), or spiral or corkscrew (spirochete [pronounced SPY-ruh-keet] or spirilla). Some bacteria also have a shape like that of a comma and are known as vibrio.
Bacteria most commonly reproduce by fission, the process by which a single cell divides to produce two new cells. The process of fission may take anywhere from 15 minutes to 16 hours, depending on the type of bacterium.
A number of factors influence the rate at which bacterial growth occurs, the most important of which are moisture, temperature, and ph.
Most bacteria require a pH of 6.7 to 7.5 (slightly more or less acidic than pure water). Other bacteria, however, can survive at a pH more severe than that of battery acid.