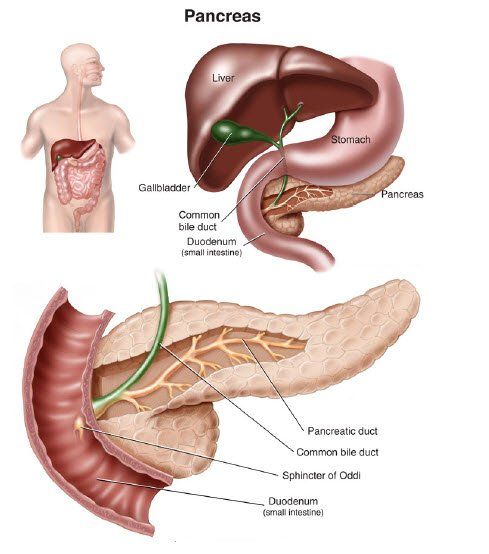
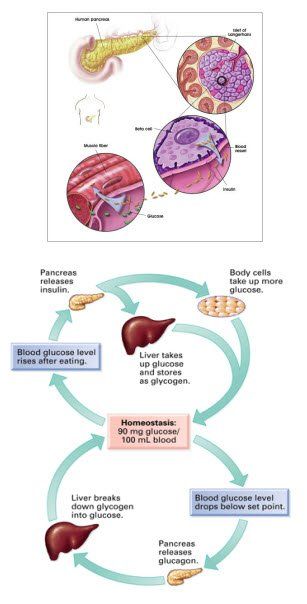
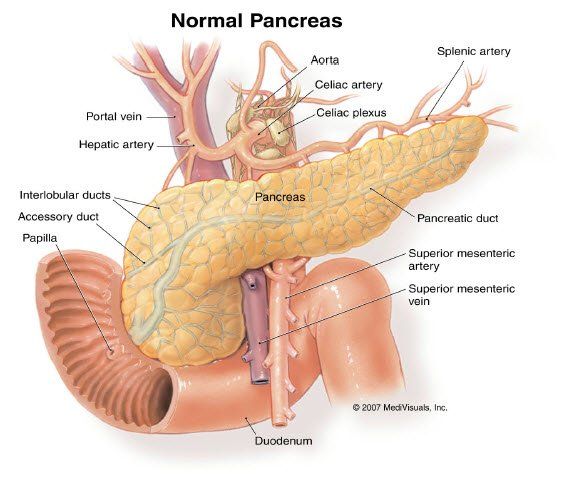
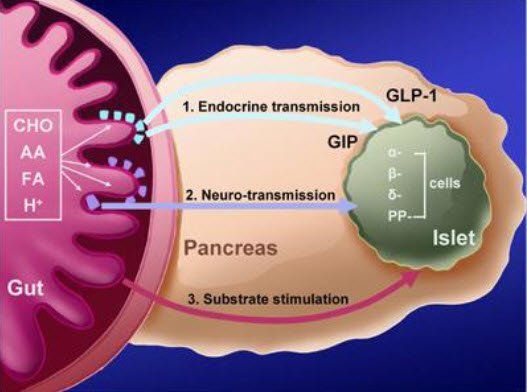
Diabetes mellitus is a disorder of metabolism that results from a deficiency of insulin, a hormone secreted by the beta cells of the pancreas. Insulin is required for the removal of sugar (glucose) from the blood by muscles after a meal and to prevent the over secretion of glucose from the liver during periods of fasting
Insulin transports glucose into the cells for use as energy and storage as glycogen. It also stimulates protein synthesis and free fatty acid storage in the fat deposits. When a person lacks sufficient insulin, body tissues have less access to essential nutrients for fuel.
An inadequate amount or inefficient action of insulin leads to elevated blood levels of glucose, the hallmark of diabetes.
This problem is made more complex by the fact that diabetes mellitus is not a single disease, but occurs in several forms, and has complications that affect virtually every system of the body.
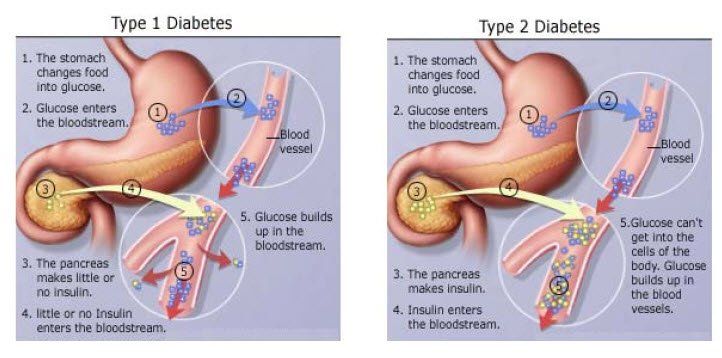
The most common forms are Type 1 (insulin- dependent) diabetes, which usually starts in childhood or adolescence, and Type 2 (non-insulin dependent) diabetes, which typically affects adults and increases dramatically with age and obesity
Other types include gestational diabetes mellitus (gdm), which occurs during pregnancy, and “other specific types” which include people who have diabetes because of a genetic defect, endocrinopathologies or exposure to certain drugs or chemicals.
New Treatments for Diabetes
Sandimmune Therapy
aims to prevent the destruction of islet beta- cells. This drugmay prevent circulating islet-cell antibodies in the blood from attacking islet cells. However, the drug can also be harmful to the liver and kidneys.
Pancreas Transplants
are an option but because of the high risk of immune rejection,people receiving a pancreas transplant must take drugs that suppress the immune system. Unfortunately, these drugs eventually can cause more problems, including infection and damage to the liver and kidneys. Patients also face a greater health risk of diabetic complications from long- term immune system suppression.
“Epidemiologic studies have demonstrated that children who acquire natural infections develop immunity to subsequent infections, with the protective effect increasing with each natural infection.”
Pediatric Infectious Disease Journal
Diabetes and Signaling
Health care is slowly changing its focus from treatment of metabolic disorders with drugs and chemicals to shifting towards procedures that restore and maintain the normal communication and control systems of the human body.
Central Nervous System & Metabolism
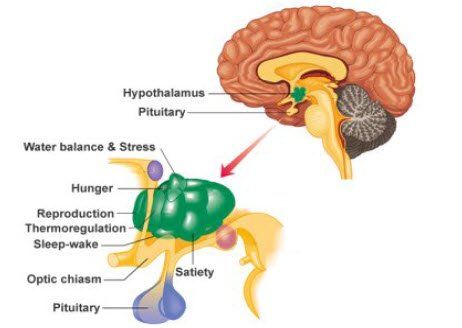
Factors such as blood sugar levels, temperature, fluid and electrolyte balance, blood pressure, and body-weight are held to a precise value called the set-point, and though it can migrate from day to day, it usually remains remarkably fixed
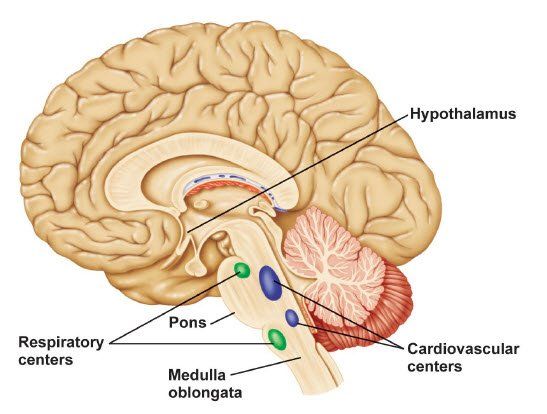
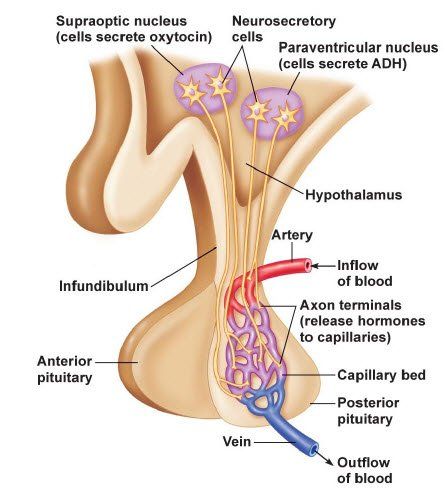
To achieve the task of maintaining metabolic balance, the hypothalamus must receive inputs about the state of the body, and must be able to initiate compensatory changes as needed.
The hypothalamus receives millions of nerve messages from complex areas of the rest of the nervous system including the nucleus of the solitary tract, reticular formation, the retinas, circumentular organs, the limbic and olfactory systems, sense organs, neocortex, osmoreceptors, as well as numerous touch receptors through the body.
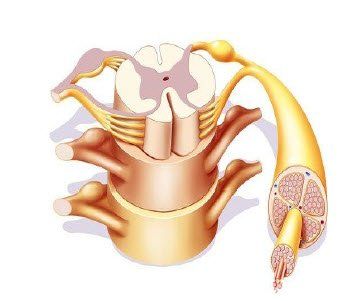
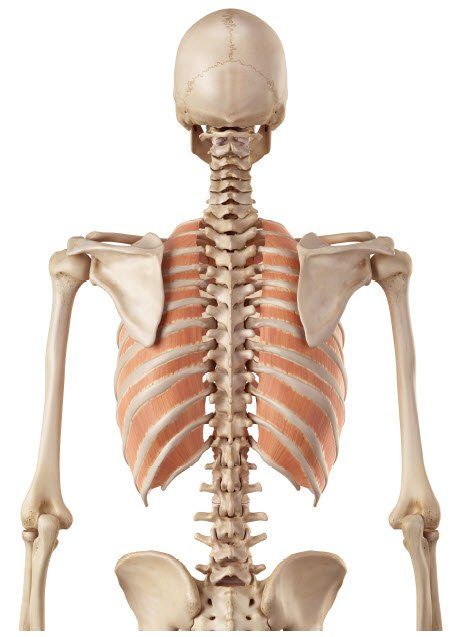
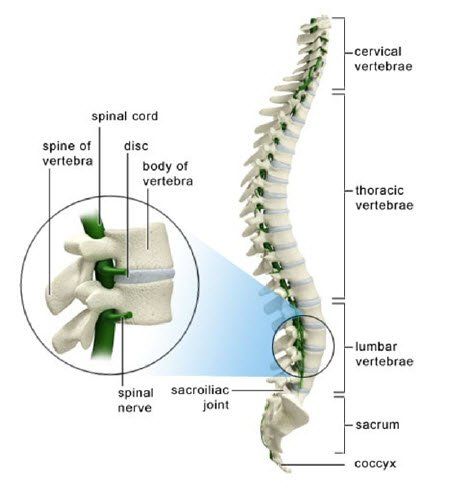
The effectiveness of the hypothalamus to control metabolism and other functions is directly related to the functional capability of the nervous system to be able to send and receive nerve messages and especially to maintain the integrity of those nerve messages as they travel along the spinal cord.
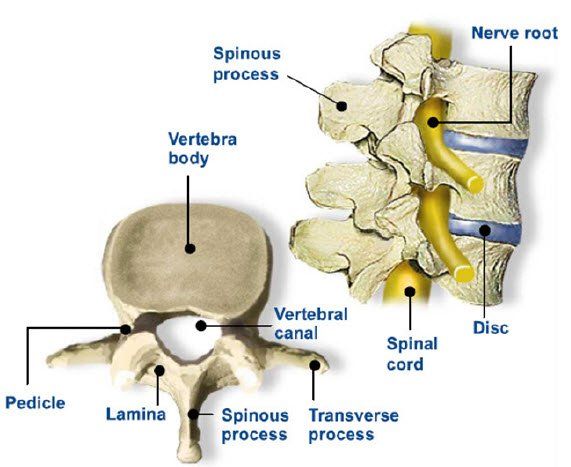
Subluxations interfere with the normal flow of nerve impulses and can cause an increase or decrease of nerve activity.
Spinal nerve interference has been documented by leading scientific researchers to be a contributing factor of endocrine and metabolic disorders including diabetes.
“Lesions of the hypothalamic input region may produce a variety of symptoms, including diabetes, obesity, sexual dystrophy, and loss of thermal control.”
Correlative Neuroanatomy & Functional Neurology
“Hyper functional or Hypo functional neurons along a neural chain prevent normal nerve transmission causing disturbances in the homeostasis of the cells, tissue, and organs.”
Dr. T.N Lee, Academy of Pain Research
Chiropractic Health Care
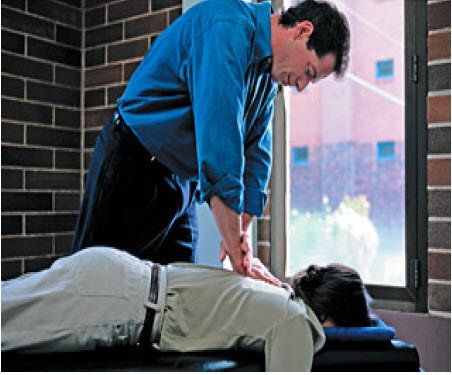
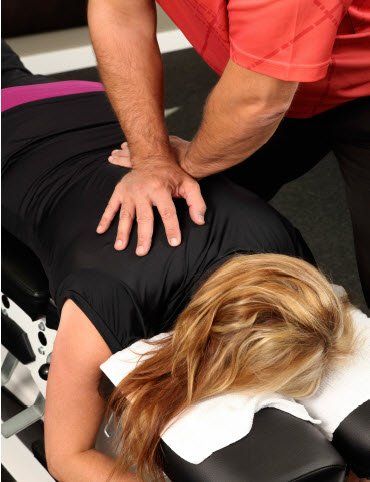
Chiropractic is a health care system that is founded on the premise that a proper functioning nervous system is essential to overall health and function of the human body. Doctors of Chiropractic detect and correct vertebral subluxations by physically adjusting the spine. This restores the nervous system to an optimum level of function, which maximizes the body’s inherent healing potential.
An investigation was undertaken to study the circumstances of life of 115 families with children aged 0-7 years suffering from asthma, diabetes, and epilepsy. Their contacts with traditional and alternative health care systems were investigated. In addition, 317 families with healthy children were also investigated. One-third of the sick children had received alternative treatment. The majority had consulted chiropractors. 73% of the parents reported that the treatment had been of benefit to their child.
National Library of Medicine
“Subluxation alone is a rational reason for Chiropractic care throughout a lifetime from birth”
Dr. Lee Hadley, Syracuse Memorial Hospital
Case Study: An 80-year-old man with a history of Diabetic Mellitus complained of low back pain along with burning pains in the lower extremities and poor balance. Joint dysfunction was detected in the mortise and intertarsal joints and myofascial trigger points were found in the quadratus plantae muscles. The patient was treated with chiropractic manipulations 18 times over a period of 4 months. The treatments brought about drastic improvements in both symptoms and clinical signs of nerve function.
Journal of Manipulative and Physiological Therapeutics
CHIROPRACTIC FACTS
Training to become a Doctor of Chiropractic requires a minimum of six years of college study and clinic internship. Training includes two years of the basic health sciences and the remaining four years focusing on the correction and prevention of spinal and structural problems that affect the nervous system.
CONCLUSION