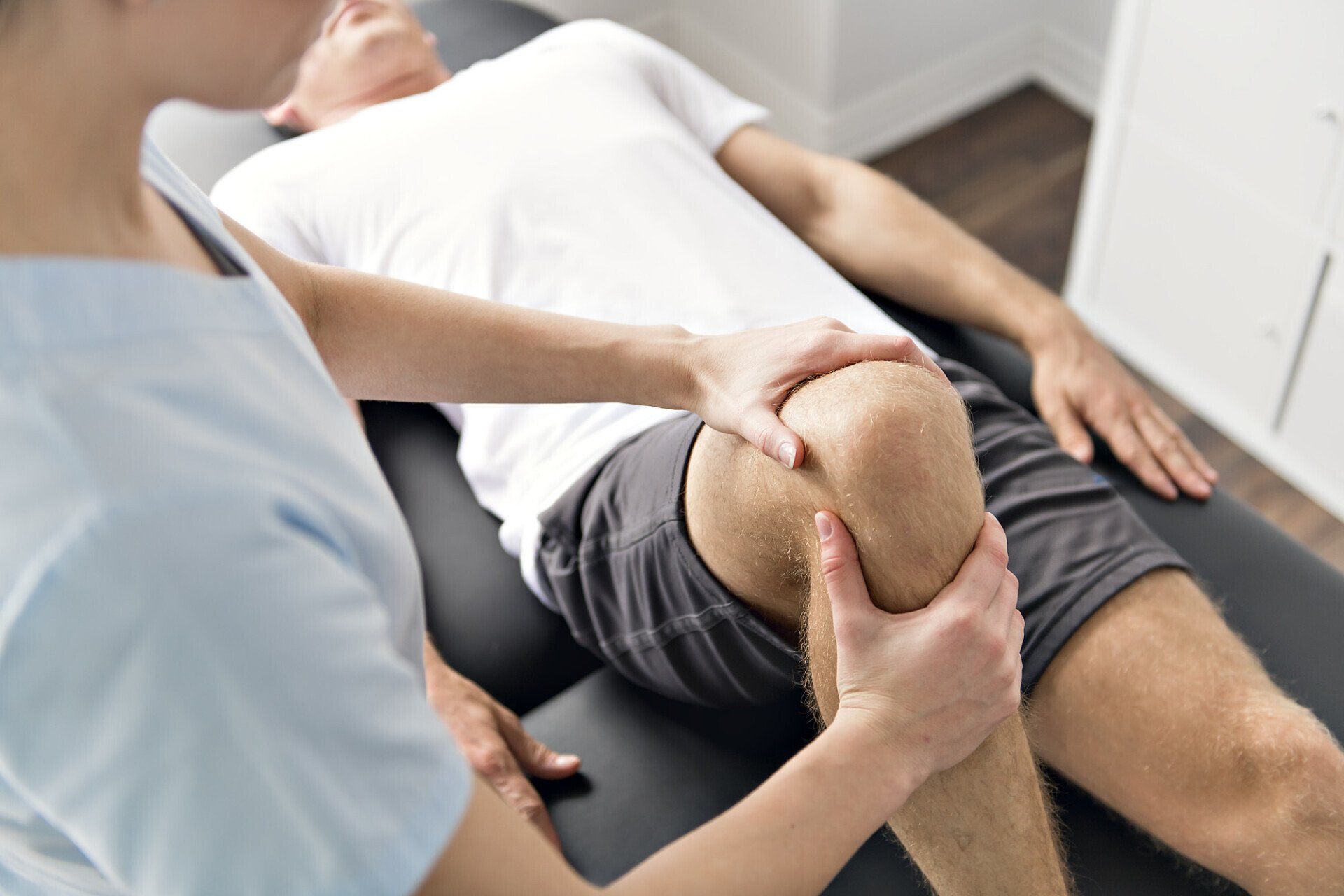
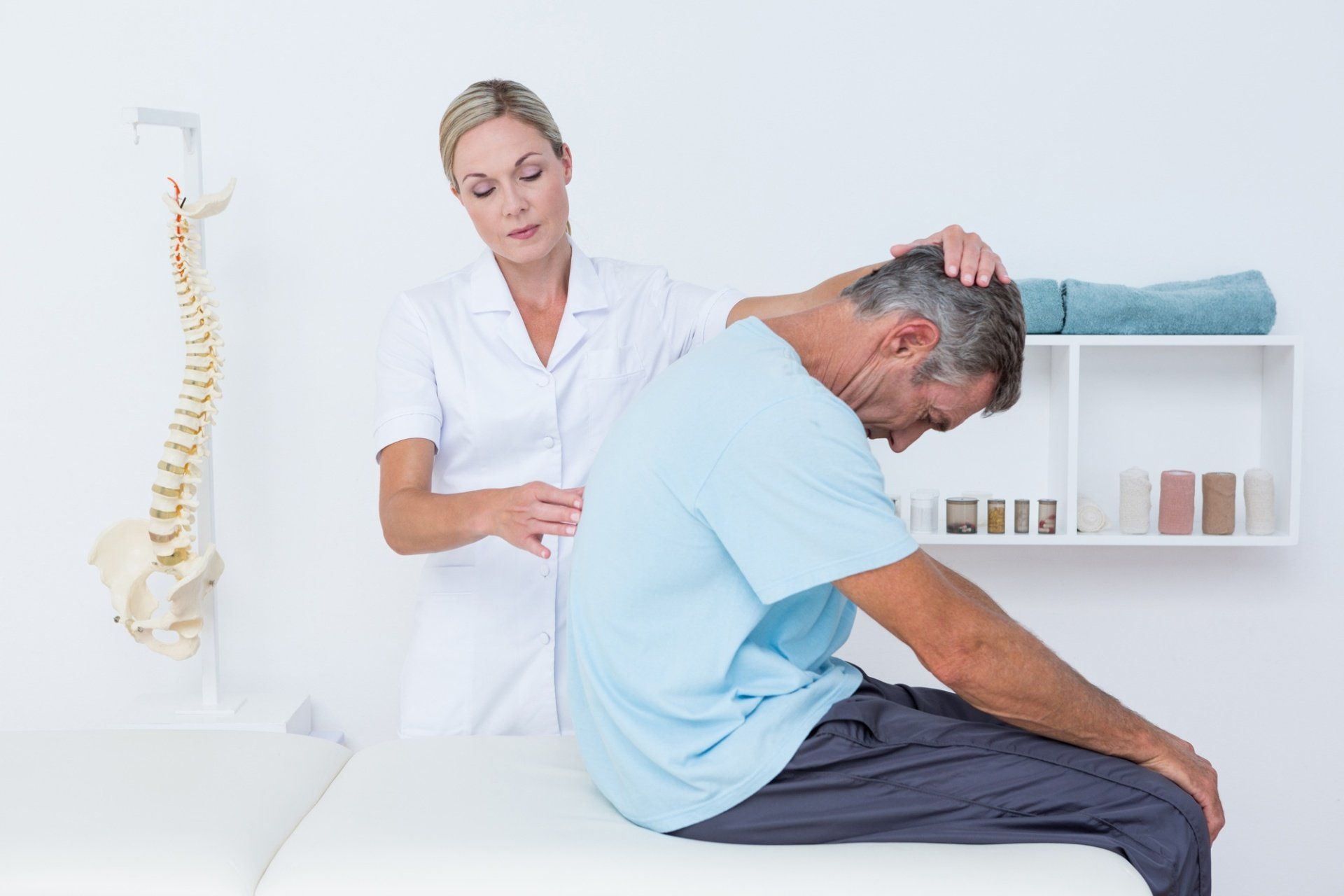
The past 20 years of health science and research has seen a tremendous increase in the knowledge and understanding of the human immune system, mostly due to cancer and AIDS research. The findings have completely changed our approach to health care as we slowly change from a disease/symptom model to one in which the function and communication of the immune system is optimized.
Nervous System Control Of The Immune System


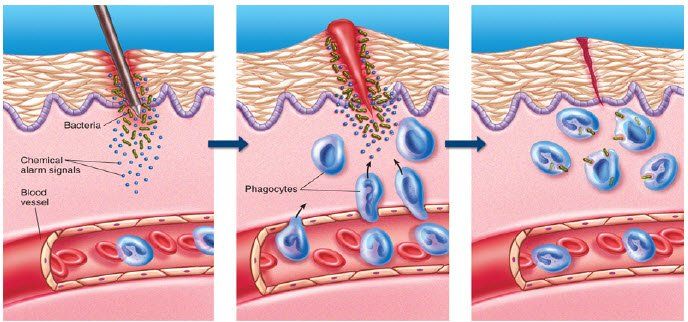
Our bodies are constantly under attack from foreign invaders such as environmental toxins, pollutants, bacteria, germs and viruses.
The immune system is our body's natural defense against these attackers. The immune system is made up of organs, structures and white blood cells whose job it is to identify and destroy disease causing organisms such as bacteria, viruses, fungi, parasites and even the body's own cells that have malfunctioned.
The immune system is divided into two components, non-specific and specific. The breakdown is for classification purposes only as there is a constant and complex interaction, coordination and communication between all parts of the immune system.
Non-Specific: also referred to as innate or non-adaptive. They are generally able to distinguish foreign antigens, but are unable to recognize specific invaders. They will respond to a foreign antigen in the same manner, despite repeated exposures.
They do not adapt and improve their effectiveness against previously encountered antigens. Non-specific components include:
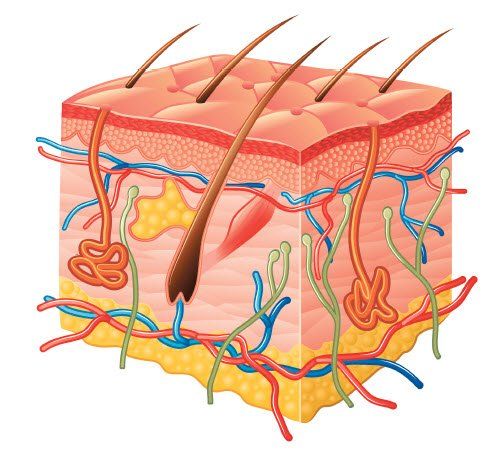
Physical Barriers: skin, mucosa, stomach acid
Chemical Agents: lysozymes complement
Effector Cells: macrophages, natural killer cells
Specific: also referred to as acquired immunity or adaptive. Is able to distinguish foreign cells from self-cells and can distinguish one foreign antigen from another. Acquired immunity cells have mechanisms for selecting a precisely defined target and for remembering the specific antigen so that subsequent exposures will result in a more effective and efficient response.
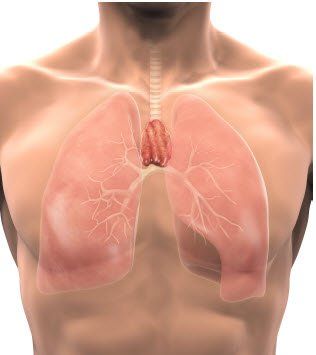
The thymus is a small, ductless gland, located in the anterior section of the chest cavity.
The thymus consists of two lobes that are connected by aeroler tissue. It is a primary lymphoid organ, and it often referred to as the "master gland of the immune system."
In the thymus, lymphoid cells undergo a process of maturation and selection prior to being released into the circulation of the immune system. This process allows T cells to develop self-tolerance (distinguishing self from non-self).
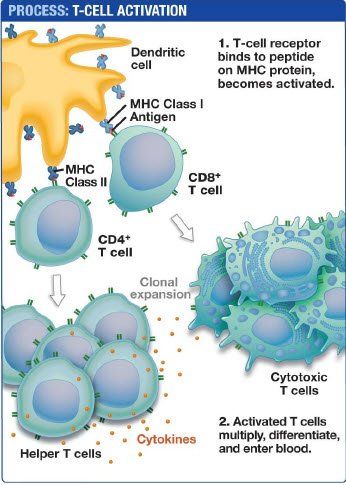
While developing in the thymus gland, any T cell that reacts to the thymus's major histocompatibility complex (MHC) is eliminated. It is estimated that anywhere from 95-99% of all T cells are eliminated during this process. T cells that tolerate the MHC are allowed to mature and leave the thymus where they circulate in blood and lymph.
The entire repertoire of T cells is approximately 1016 with each T cell having as many as 100,000 receptor sites on its surface. T cells are classified as cytotoxic or killer T cells, suppressor T cells, and helper T cells, which are further, classified as Th1 and Th2 helper T cells. The proper balance and ratio of these various T cells are critically important in maintaining proper immunological function.
"The thymus derived lymphocytes or T cells are pivotal to the control and homeostasis of the immune system."
QMC~ Institute of Infection and Immunity
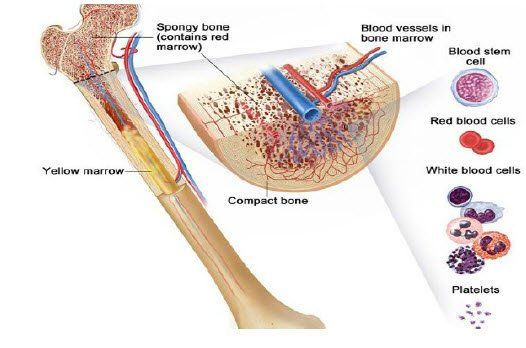
Modern textbooks of disease and anatomy all stress that the gland undergoes fatty involution with age in man, but omit reference to the statements here and there in the literature that the gland is active and produces lymphocytes throughout life.
To suggest that bone marrow, which also builds up fat throughout life, is atrophic and not important to adults, we would have to deny all modern hematological concepts.
- increasing key immune signals called lymphokines or cytokines.
- causing greater number of T cells to develop IL-2 receptors more rapidly.
- increasing rapid white blood cell proliferation and activation.
- preventing tissue wasting that occurs with thymus gland atrophy.
- reduces and controls autoimmune reactions.
- preventing bone marrow injury and blood cells reduction following cancer treatments.
- increasing disease fighting antibodies, yet reducing the level of "allergic antibodies".
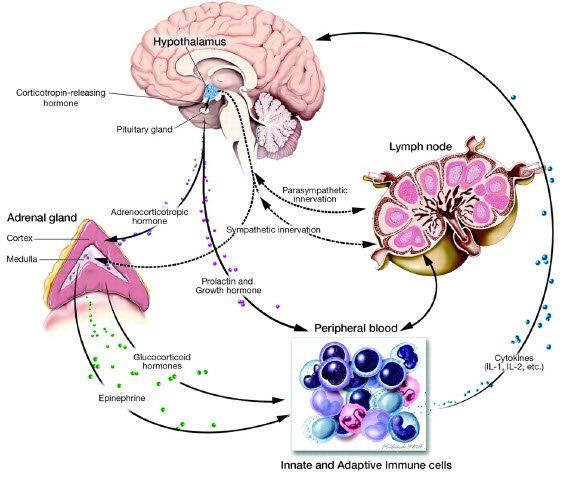
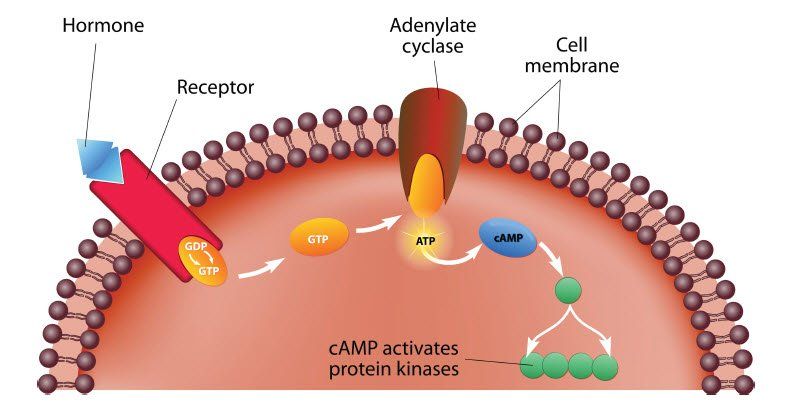
This connection or communication pathway is also mediated via the bloodstream, and therefore involves hormonal communication. The term hormone not only signifies classical endocrine systems, but also molecules released by the nervous and immune systems which have functional effects from some distance.
Thus, the brain and the nervous system are part of a neuroimmuno-regulatory network in which each of the various components not only communicate with each other, but also regulate additional sites in the body.
There are two main pathways that connect the brain and the immune system, namely the autonomic nervous system, (made up of the sympathetic and parasympathetic components), and the hypothalamic-pituitary-adrenal-axis (HPA). In order for the two systems to influence one another, they must have a mechanism by which to communicate. The main type of communication is mediated by chemical messengers which are released by nerve cells, endocrine organs and immune cells.
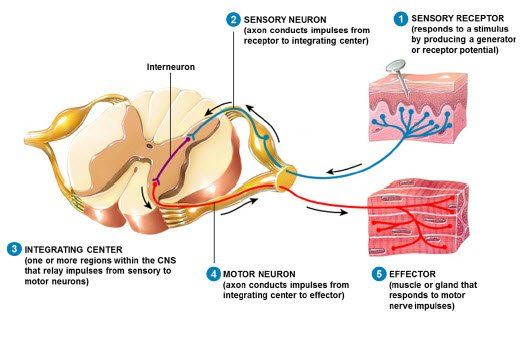
The immune system is composed of lymphoid tissues, and the fact that these tissues are innervated with sympathetic nerve fibers adds support to the evidence that the central nervous system directly influences immune function. Not only do nerve fibers form neuro-effector junctions with lymphocytes and macrophages, but certain neurotransmitters secreted from these nerves are able to have effects on distant blood cells.
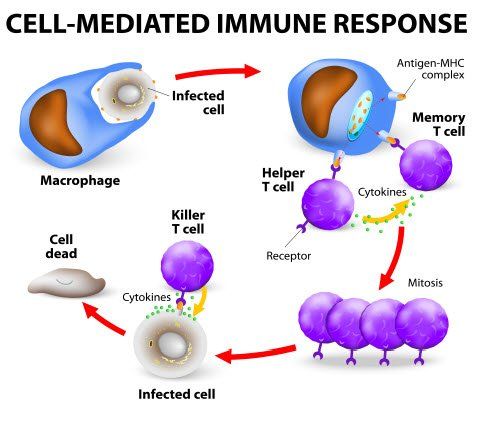
In addition, specific receptors for several neurotransmitters have been detected on T cells, B cells, and monocytes. Thus, the nervous system is able to:
- Induce T cell function, including cytokinesecretion, proliferation, integrin-mediatedadhesion and migration.
- Modify T cell membrane potential andthereby affecting the gating of specificvoltage gated channels.
- Modulate antigen driven, CR mediated, Tcell function.

Immunologists at Oregon State University have recently uncovered some important clues as to how the immune system works at a fundamental level. The key, scientists say, is understanding how some of the T cells, which are sort of the quarterback of the immune system that directs other cells to go do their dirty work, can get stimulated to do their work even better, or tone it down in the case of an autoimmune conditions.
One of the things that have intrigued scientists is the apparent correlation between inflammation and a dysfunctional immune response, especially with autoimmune diseases. Steroid treatments, for instance, which have strong anti-inflammatory effects, are often used to treat autoimmune disorders. "But using a powerful steroid drug, which can have many side effects, to indirectly affect something as delicate as the immune system is like hitting an ant with a sledgehammer", according to Anthony Vella, an assistant professor of microbiology at OSU. "What we have tried to identify is exactly how the process of inflammation is related to immune function and what cellular processes are involved." In one recent breakthrough, the OSU research program determined that inflammation in conjunction with the activation of other T cell stimulatory molecules can help T cell growth and increase the number of "fighting" T cells. In experiments, OSU researchers showed that injecting mice with an antigen caused significant death of the antigen-responsive T cells; however, when

inflammation was present, it prevented the death of these cells. In cell membranes of certain bacteria, there is a natural bacterial lipid called lipopolysaccharide, or LPS. It appears that LPS can play a role in causing inflammation, and keeping activated T cells alive. OSU researchers have also shown that the LPS inflammatory signal, which prevents T cell death, is dependent upon IL-1 and TNF stimulation of IL-6. This result is of interest beyond immunology, since IL-6 is a major factor involved in neurological function. Vella speculates that there may be a potential link between nervous system and T cell survival.
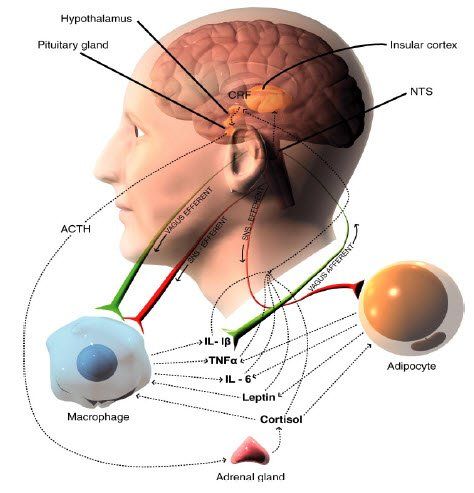
There are four major categories of cytokines:
Interferons, so named because they interfere with replication. The major types of interferon are: Interferon Alpha (IFNa) Interferon Beta (IFNb) Interferon Gamma (IFNg)
Colony Stimulating Factors (CSF), support the growth and differentiation of various elements including the bone marrow which regulates the differentiation of bone marrow stem cells.
Tumor Necrosis Factor (TNF), plays a major role in inflammatory response and cell apoptosis.
Interleukins, which is the largest group of cytokines and are so named because their fundamental function is the inter communication between various populations of white blood cells.
The range of cytokine effects have found to be far wider with the recent discovery of small proteins that influence the migration of cells and attract them to the sites where they are needed.
This process is called chemotaxis; the cytokines that emanate from sites of damage to bring in these cells are the chemokines.
"In the absence of cytokines for the helper T cells, the remainder of the immune system is almost paralyzed."
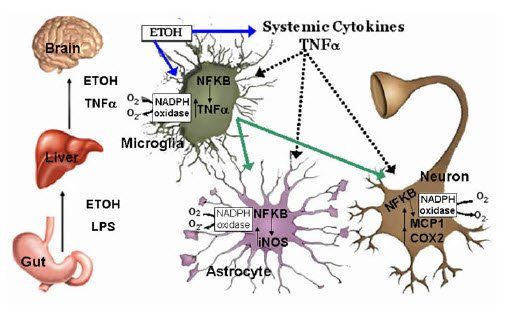
The importance of the cytokines in the host response to injury, invasion and infection can scarcely be overstated. Without them, the body's ability to fight off pathogens, repair damage, and maintain health would be seriously impaired and far less effective. Full protection against disease, injury, and even the normal wear and tear of living requires the participation of many different bodily systems. It is the cytokines that orchestrate, coordinate and integrate them.
MECHANISM OF HORMONE ACTION
The immune system is so complex in its relationship to organs, glands, and cells that immune dysfunction and immune suppression can create a drastic negative effect on the entire health and homeostasis of the body.
The thymus gland and T cell function play such a pivotal and important role in generating and regulating immune response that a deficiency or imbalance in their function will cause immune system dysfunction or suppression to occur.
Much of the increase has been due to the aggressive and invasive approach of treating symptoms with medication, as opposed to restoring and maintaining the proper function of the immune system. Among the manifestations of immune disorders include
Autoimmune, in which the cells of the immune system confuse normal body cells with foreign antigens and attack them. Autoimmune disorders include: rheumatoid arthritis, asthma, allergies, lupus, diabetes and multiple sclerosis.
Immunodeficiency disorders are characterized by a weak immune system response and are often associated with chronic infections. They include Epstein-Barr, AIDS, viral infections, otitis media, and even cancer may result from immune suppression.
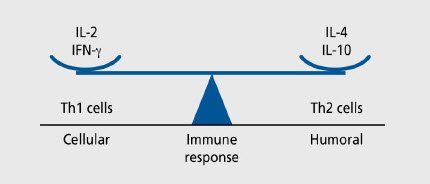
Th1 and Th2 lymphocytes and their characteristic cytokines possess opposite roles in the regulation of the immune system. Th1 cytokines participates mainly in the regulation of the cellular defense while Th2 lymphocytes activate B cells and regulate the immunoglobulin synthesis and switch via their characteristic cytokines.
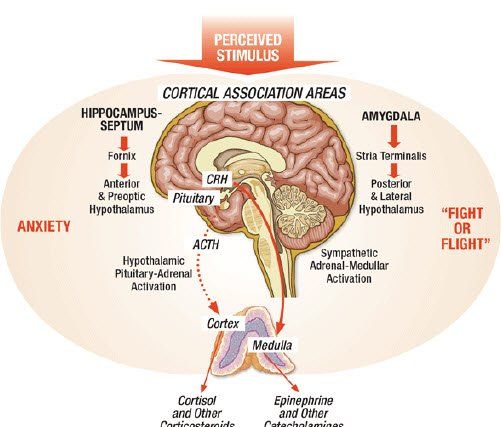
Substantial research has clearly demonstrated that a wide range of stress can deplete immune system resources and adversely affect neurological and biological communication resulting in abnormal levels of B and T cells, decreased responsiveness of natural killer cells, and fewer IgA antibodies to be secreted in the saliva.
Stress can be defined as "a state of disharmony or threatened homeostasis provoked by psychological, environmental, and physiological stressors.
Stress is also invoked as an important part of the normal response to stimuli and should not be thought of as an abnormal reaction since it involves the "fight or flight" principle.
Much of this response is mediated through the hypothalamic-pituitary pathway and is integrated in the hypothalamus to monitor and control certain functions such as the sympathetic nervous system and endocrine system.
Although stress is generally associated with negative connotations, it is a double-edged phenomenon. The body would not be able to survive without the acute stress response, as it prepares the body for short, emergency responses to potentially life threatening situations.
However, a lingering stress response to non-emergency situations is bad and can lead to chronic health conditions. Stress becomes a hazard to the body when the communication systems of the body are interrupted or overwhelmed by a variety of physical, chemical or emotional stressors.

Types and Causes of Stress
Physical: The primary cause of communication breakdown is nerve interference in the spinal column. When the spine is in its proper, structural position, it protects the nerve pathways and allows the nervous system to send and receive information.
However, because the spine is moveable, it is also susceptible to various physical stresses and forces which can cause the spinal vertebra to lose their proper, structural position. These spinal misalignments cause abnormal reflexes, loss of normal mechanoreceptor function, and nerve interference which reduces the overall effectiveness of the communication of the body.
Chemical: There are more drugs designed to treat and suppress components of the inflammatory response than any other single category in the world, in fact there are more drugs whose primary purpose is to inhibit the normal communication of the nervous and immune system than all of the rest of the drugs combined.
Drugs may result in a temporary reduction of symptoms, but they do little to improve and optimize the actual healing process and often lead to dangerous side effects and immune system disorders.
Antibiotics have become a popular weapon in the medical arsenal against disease. Although no one would argue with the appropriate use of antibiotics, there is a tremendous volume of research which clearly demonstrates that antibiotics have been grossly overused resulting in weakened immune systems and stronger bacteria and foreign microbes.

Emotional: There is an abundant body of scientific research to support the concept that emotional stress has a negative impact on the immune system. Thoughts and emotions can trigger complex chemical reactions that affect multiple body systems and particularly the immune system. Periods of intense emotional stress can result in decreased levels of natural killer cells, sluggish killer T cells, and diminished macrophage activity.
"Pressed by patients and advancing technology, health care will soon change its focus from treatment to enhancement, from repair to improvement, from diminished sickness to increased performance. The transformation has already begun. Accompanying this will be an increased emphasis on psychoneuroimmunology, the science that deal the minds role in helping the immune system to fight disease. Which will become a vitally important clinical field-perhaps the most important field in the 21st century."
Michael Crichton, M.D.
Recent Articles

Blogs and Articles